Emergency medicine is in a state of crisis throughout the country due to overcrowding and ever lengthening wait times. Due to the Affordable Care Act, the demand is only expected to increase as health insurance becomes more readily available. The basic operational concept of an Emergency Department (ED) is that the clinical resources are available when needed. It sounds simple enough, but hospital administrators continue to list ED patient flow as one of their primary challenges, so much so that the Institute of Medicine now considers ED crowding a public health concern. Long wait times in reporting EDs have grown twice as much as the increased volume according to the 2012 Annals of Emergency Medicine. Mortality rates in crowded EDs were higher than EDs not perceived as being crowded. Medical and clinical staff response time degrades exponentially as utilization approaches 100%, and common sense aligns with reality in that patient satisfaction decreases linearly as Length of Stay (LOS) times increase. These inefficiencies contribute to a poor work environment, which can lead to adverse patient outcomes.
More than just patient and staff satisfaction, long LOS also reduce an ED’s financial success. For every instance of Left without Being Seen (LWBS), a hospital loses revenue, which, for a 50,000 visit/year ED, can equate to $500,000.00 annually. Additionally, an inefficiently operating ED affects the entire hospital since it is often responsible for 50% or more of annual admissions.
Improving efficiency and reducing cost within the ED presents unique challenges due to the perceived variability in volume and acuity. However, the demand curves within EDs are predictable and not unique to a particular system or region.[1] The predictability extends to acuity levels and LWBS rates based on wait times. Three stages of operational efficiency require investigation: Input, Throughput and Output. These stages have a high amount of variation depending on the operational model implemented.
The traditional ED operates in a linear fashion. Patient arrives, registers and waits until a room becomes available. This creates bottlenecks and doesn’t account for demand or acuity variability. The following models present some flow improvement solutions and best practices.
Split Flow
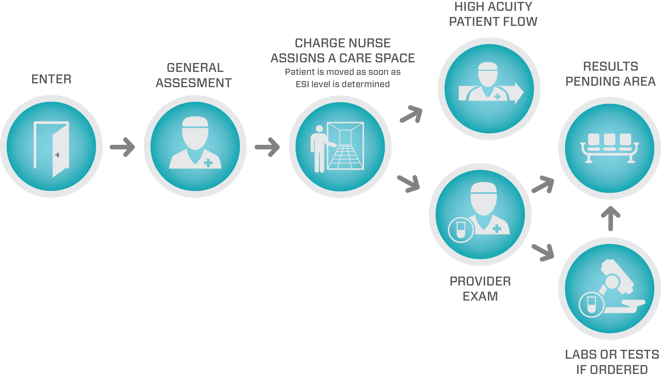
In a split flow model, a nurse, Nurse Practitioner (NP), Physician Assistant (PA) or provider sees patients and performs an initial assessment to assign acuity level. The split flow is most efficient when there is a high volume of Emergency Severity Index (ESI) Level 3 patients. The charge nurse, using medical protocols as the determining factor, then assigns a care space and the patient is registered. Next, the provider performs an examination then orders initial labs, tests, medications, etc., before moving patients to the results-pending area. The results-pending area is a place where patients can receive medications and wait for lab results. These areas, which should have a clinician on staff to ensure safety, improve the ED’s ability to process new patients more quickly and allow for more efficient bed turnover.
However, EDs that experience long LOS, high LWBS rates and have opportunities for improvement across all acuity levels (ESI 1 to 5) can benefit from the split flow model. Split flow models have the ability to achieve a 35% improvement in LWBS patients and, on some days, the split flow model’s vertical pathway processes 60% of patients.
Provider-in-Triage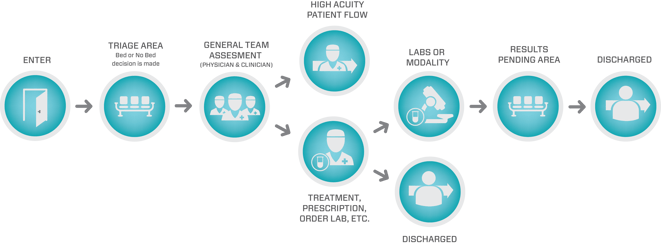
The Provider-in-Triage (PIT) method places a provider in the triage area to examine and treat low-acuity patients quickly. This model, particularly effective in EDs with high daily volume and high numbers of LWBS, low-acuity (ESI 4-5) patients, only requires the inclusion of a small, private workspace, basic tools and a clinician to team with the provider to treat patients. After assessing the patient, the provider can take all appropriate care steps and discharge the patient, or divert them to reception if their assessment determines other factors requiring further testing or treatment.
Research performed by Academic Emergency Medicine showed that adding a PIT helped reduce the LOS. However, further study revealed that relocating the provider into a PIT model from fast track actually increased the LOS.
Fast Track 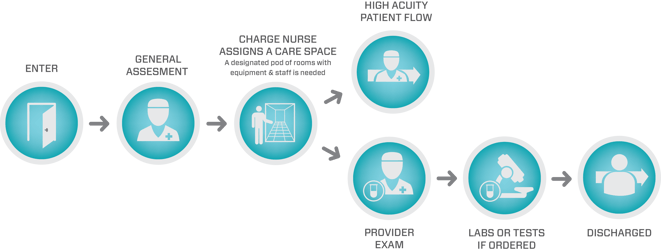
The fast-track model is ideal for EDs that also have high daily volumes and LWBS patients, but whose patients are low-to-middle acuity (ESI vertical 3, 4 or 5) with prolonged LOS. This method works well in EDs where the high volume times are generally known. Supporting service lines, such as radiology and laboratory testing, can be scheduled enabling staff to test and treat mid-level acuity patients more quickly, which in turn reduces LOS and improves throughput metrics. To successfully implement this model, a dedicated care area, as well as clinical and medical staff (whether physician, PA or NP) with assigned equipment is necessary.
No matter which model an ED utilizes, there are still operational bottlenecks outside the ED, as it is dependent on multiple departments to move through the Input, Throughput and Output stages of the process. If, for instance, Registration is backlogged, patients aren’t able to get past the front desk into the system. Even something as simple as patient transport services can affect throughput. Working with an Organizational Transformation consultant to perform an in-depth study of the admission process will help to understand where bottlenecks occur. Improving patient flow and avoiding administrative roadblocks within the admission process, prevents the ED from becoming an inpatient waiting room.
When it comes to the spatial layout of the ED, one model doesn’t fit every situation. The ideal layout for a high-volume, high-acuity ED will differ from a low-volume, low-acuity ED. An efficient spatial organization for an urban ED will be different from a community-based suburban ED or a freestanding ED. To obtain the greatest efficiency, the physical environment needs to respond to acuity ranges, census demands, staff workflows among other factors.
[1] “Cracking the Code: Fixing the Crowded Emergency Department, Part 2: Creating the Analytic Model,” CommonSense, November/December 2013.
This post was written by former Array employee, Dwight Young.