Originally featured in Imaging Economics
Building an IR suite is a major investment. Smart planning can help ensure a successful project. Hospitals make a considerable investment when developing an interventional radiology (IR) suite. While the cost of constructing a new room can exceed $800,000, constructing a new suite can involve an expenditure of $2.5 million, perhaps more. These hard costs must be added to the cost of imaging equipment, which can range from $1.5 to $2.5 million, depending on the features desired, and, of course, the buying power of the facility. When an organization is considering the addition of an IR suite, health care leaders must explore and research what is required to maximize their investment. Here are some measures to consider for strategic planning.
What Is Interventional Radiology?
IR—or, as it is sometimes referred to, vascular and interventional radiology—began in the 1970s as an alternative to more invasive surgical procedures. Today, IR is an accepted subspecialty of radiology. IR procedures in common use include angioplasty, stent placement, chemoembolization, and biopsy. Hospital administrators, architects, and health professionals who are considering adding an IR suite, or expanding their existing suites, must consider several key issues related to the design of this increasingly important hospital function. Visit Array's project section for a feature on Nemours/Alfred I. duPont Hospital for Children's Hybrid Suite.
Understanding the Professionals Involved
A fairly large contingent of health professionals can be involved in IR suite operation. Traditional radiologists, interventional radiologists, vascular radiologists, cardiologists, electrophysiologists, anesthesiologists, surgeons, and nurses may all have roles in the IR suite. Understanding each user's role and needs is crucial for the architect or designer; even more crucial is a grasp of the "turf" issues involved. Facility management personnel will certainly play an important role in the design process. However, a successful project includes the input of the health professionals who will ultimately work in the IR suite. Satisfying and balancing everyone's different needs, desires, and idiosyncrasies requires tact and diplomacy on the architect's part. This is a primary reason to consider retaining the design professionals at early decision points in the process.
The Hospital Administrator's Role
The various health care team members often bring conflicting requirements that can be managed only by thoughtful leadership from hospital administration. Power struggles can occur, and the hospital administrator (or their designee) must carefully balance everyone's wants and needs. The architect alone, or even in conjunction with a facility manager, cannot fulfill this role; the hospital administrator must act as the team leader and set the project tone and parameters.
The IR Suite's Unique Design Issues
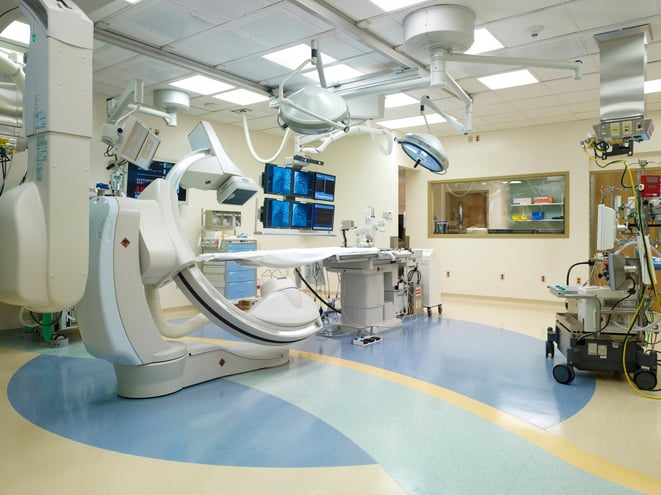
During the planning and design process, several issues will impact the IR suite. Equipment location, vibration, HVAC, and radiation exposure all require special consideration. Equipment placement within the suite is crucial. Each medical discipline requires a distinct set of equipment. The various procedures share common imaging equipment. These include the biplane (frontal, which is floor-mounted, and lateral, which is ceiling-mounted) imaging arms, the imaging table, and the fluoroscopy imaging monitors. Each procedure can require a variety of additional equipment that includes:
- electrophysiology systems
- hemodynamic equipment
- anesthesia machines
- perfusion systems
- surgical instrument tables
- ultrasound equipment
All of the equipment needs to be readily available when needed and out of the way if it is not. The biplane equipment often has a built-in collision avoidance system so that the image intensifiers, flat panel detectors (FPD), and the table don't "crash" into each other. A collision avoidance system, however, does not exist to prevent crashing into surgical lights, anesthesia machines, booms, columns, or any other piece of equipment. Conflicts as to their location and placement will arise. Everything should be as close as possible to the patient. Finding compromise locations that still allow for optimum use of that equipment can be a challenge; the teamwork mentioned above will come into play.
There are certain components that are common to all users
Because the frontal and lateral C-arms are sensitive, the IR suite must be protected from vibration. Often, vibration sources are generated from within the hospital. For example, mechanical fan units in proximity to the lab have been a primary contributor to unwanted reverberation. Eliminating vibration at the source is the preferred approach, though sometimes that is not possible, and other vibration isolation techniques may be required.
Radiation exposure is a constant issue in any area where radiation is used. Medical personnel in the room during procedures wear lead aprons for protection. The room walls, floor, and ceiling must offer radiation protection for anyone outside the room. This can be accomplished in several ways. Distance, mass, and duration are the main factors in determining the amount of constructed radiation protection that is needed. The architect provides the radiation safety physicist with dimensions, and identifies construction materials and the intended use of surrounding areas. The physicist uses this information, together with the equipment vendor's radiation scatter data, to calculate the shielding required to restrict radiation exposure outside of the room. The radiation safety physicist is the authority to calculate what shielding is needed. The mass of floor and wall construction may be sufficient to shield the room. If it is not, lead-lined drywall is generally used to increase mass for the necessary shielding.
Many IR procedures can be lengthy. Additional cooling, to provide lower room temperatures, may be required in the IR suite. This is partially due to lead apron use. Hours in lead aprons can affect personnel comfort and performance. More importantly, in some cases with anesthesiology, lowering room temperature is a method of controlling patient metabolism, which in turn relates to successful anesthesiology. The need for lower room temperatures must be evaluated for each installation. Of the available imaging systems, the biplane unit has particularly rigid vertical space requirements.
To accommodate a biplane, a ceiling height of between 9'6" and 9'9" is required depending on the imaging vendor. Creating that ceiling height within an existing medical complex can be difficult. Existing plenum spaces (space between the ceiling and structural floor above) may be cramped and usually contain numerous ducts, electrical conduits, and other mechanical equipment. Medical centers constructed with an interstitial floor make the insertion of an IR suite much easier, but unfortunately, these are not common in older facilities. The architect and engineering consultants will have to use ingenuity to integrate medical equipment, structural supports, HVAC systems, and enough space for staff to safely circulate around equipment. Cabling, wiring, and hoses, all part of modern medical equipment, should be off the floor to eliminate tripping hazards. Careful placement of each piece of medical equipment is necessary; adequate vendor oversight during equipment installation is crucial.
Ensuring Success
The design of an interventional radiology suite requires special consideration. For the hospital administrator, managing the team process is essential. For the architect, design will require balancing the spatial and equipment needs of different medical disciplines. Only with medical professionals' input can a state-of-the-art interventional radiology suite be successfully designed and constructed.
Blog authored by Jack Kerr, AIA. Jack retired from Array June, 2015.